By Melanie Dempsey
With 54,000 skilled and dedicated professionals, West Virginia’s hospitals stand as guardians of health care access across the state. They deliver critical care around the clock, every single day, regardless of circumstances.
Hospitals are the backbone of their communities, providing essential and life-saving services residents rely on close to home. West Virginia community hospitals offer a full continuum of care, from emergency and trauma services to maternity care, diagnostics, chronic disease management and specialized treatments, ensuring patients do not have to travel long distances to receive the support they need. Hospitals also serve as centers of expertise, coordination and stability, bringing together skilled professionals, advanced technology and critical resources under one roof.
Despite the vital role they play in their communities, West Virginia hospitals face significant financial pressures, largely because their funding depends on the insurance providers of the patients they serve. In West Virginia, as the chart below shows, hospitals face added strain because fewer residents have employer-sponsored insurance.
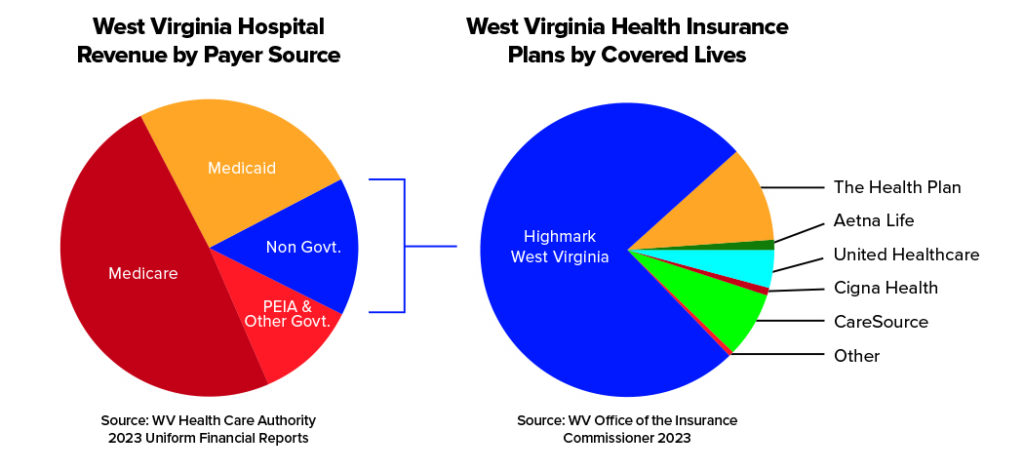 Health insurance programs differ significantly in how they reimburse providers. Employer-sponsored plans and government programs pay at different levels, with government programs typically paying below the cost of care. In West Virginia, this challenge is even more pronounced. Nearly 80% of hospital patients are covered by governmental payers, compared to a national average of about 40%. Because these programs do not cover the cost of care, employer-sponsored insurance must pay more to offset the shortfall and effectively subsidize government programs.
Health insurance programs differ significantly in how they reimburse providers. Employer-sponsored plans and government programs pay at different levels, with government programs typically paying below the cost of care. In West Virginia, this challenge is even more pronounced. Nearly 80% of hospital patients are covered by governmental payers, compared to a national average of about 40%. Because these programs do not cover the cost of care, employer-sponsored insurance must pay more to offset the shortfall and effectively subsidize government programs.
It’s important to recognize that having coverage is not the same as using services, which is referred to as utilization. Government programs predominantly serve seniors, individuals with chronic illnesses and people with disabilities. Consequently, these beneficiaries access services more frequently than the generally healthier working-age adults enrolled in employer plans. This utilization pattern naturally intensifies the financial imbalance hospitals must navigate.
Providers face an additional challenge as Medicare, Medicaid and many employer-sponsored health plans are shifting their payment models to emphasize quality and population health. This shift creates complexity in West Virginia, where residents face significant health challenges rooted in socioeconomic factors and limited access to preventive resources, among other issues.
Understanding these realities helps explain the severity of the health challenges the state continues to face. West Virginia struggles with some of the nation’s most pressing health concerns. The Centers for Disease Control and Prevention data shows the state has the highest obesity rates nationally, while the American Lung Association reports the country’s highest adult tobacco use at 21%. Diabetes and opioid use disorder also affect West Virginians at disproportionately high rates. These conditions reflect broader systemic issues, including poverty, food deserts, educational barriers and limited wellness infrastructure. Improving these measures will require continued collaboration across the state.
As reimbursement becomes increasingly linked to health outcomes, West Virginia hospitals face heightened financial vulnerability for conditions largely shaped by factors beyond clinical care. While hospitals provide essential treatment and education, lasting improvements require addressing the underlying social determinants of health.
In addition to these insurance payment challenges and population health concerns, hospitals are confronted with ongoing workforce shortages, supply chain instability, rising tariffs and policy decisions that frequently fail to account for on-the-ground realities. Hospitals serve as major economic drivers, providing skilled jobs that anchor local economies. These positions require extensive education and training and cannot be outsourced or replaced with emerging artificial intelligence. National workforce shortages force hospitals to offer competitive salaries to attract and keep qualified staff. West Virginia hospitals face a distinct disadvantage here: their heavy reliance on lower-paying government insurance limits the revenue available to compete for talent, making recruitment and retention even more difficult.
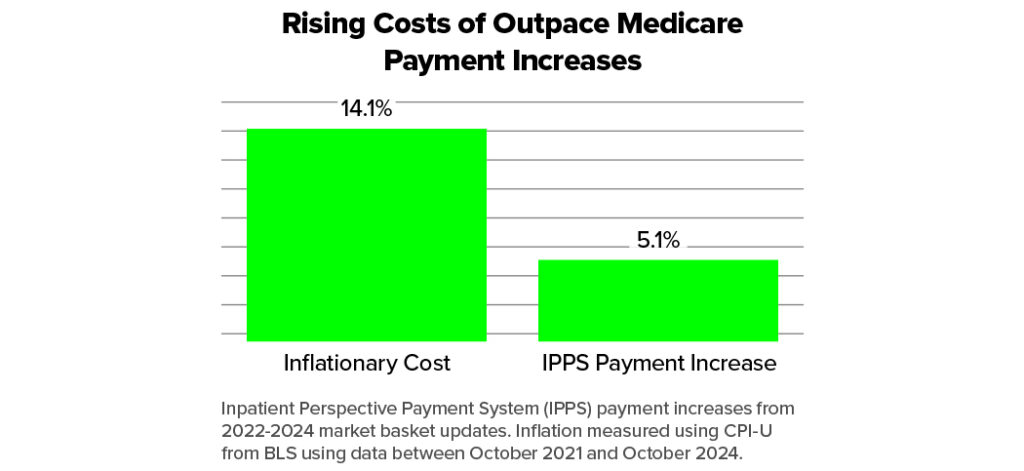
At the same time, payments have not kept pace with rapidly rising expenses. From 2022 to 2024, general inflation rose by 14.1%, yet Medicare net inpatient payment rates increased by only 5.1% during that period according to The Cost of Caring: Challenges Facing America’s Hospitals in 2025 by American Hospital Association. Overall, Medicare payments currently cover only about 80% of the cost of providing hospital care, leaving hospitals responsible for the remaining shortfall. The combination of escalating labor costs, skyrocketing pharmaceutical costs, persistent inflation, operational disruptions and inadequate payments threaten the long-term sustainability of hospitals and the essential services they provide to their communities.
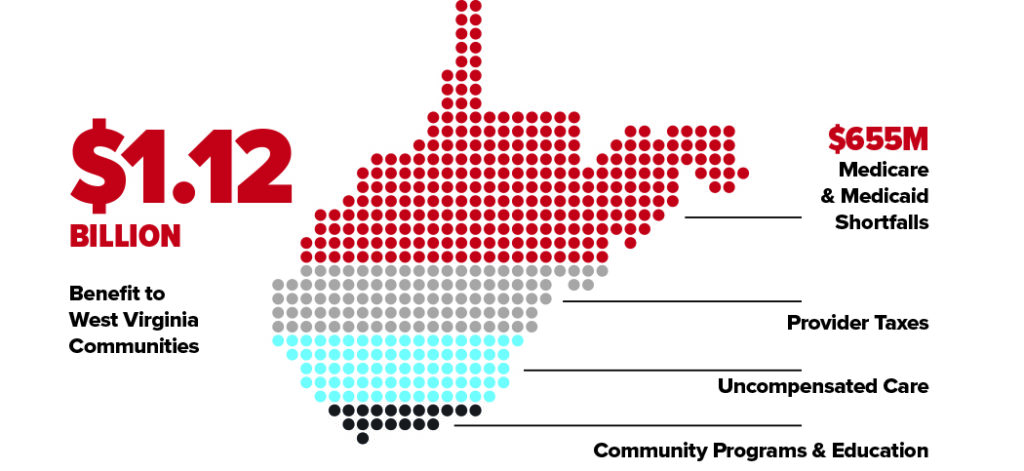
Despite ongoing financial pressures, West Virginia hospitals remain deeply committed to their communities, investing nearly $1.12 billion annually in community benefits. This includes state taxes; unreimbursed costs from Medicare, Medicaid and PEIA shortfalls; community health and education programs; charity care; and uncompensated care expenses.
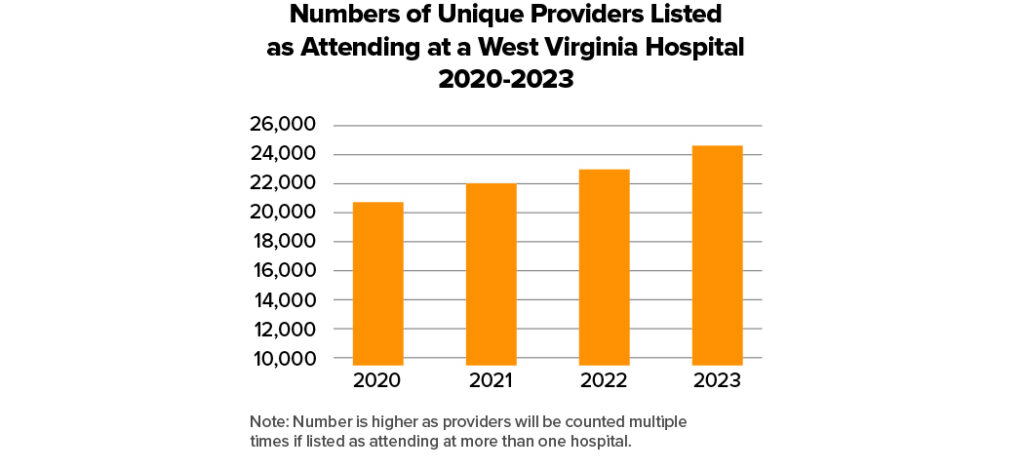
 Community benefit activities extend far beyond financial support. Hospitals work to reduce health care costs by offering preventive screening services, promote public health through wellness and nutrition initiatives, educate and train the next generation of medical professionals and conduct vital research aimed at preventing and treating disease. Even with national shortages, West Virginia hospitals have been able to expand the number of providers by nearly 20% between 2020 and 2023. These efforts reflect the hospitals’ enduring mission to strengthen the health and well-being of all West Virginians, regardless of ability to pay.
Community benefit activities extend far beyond financial support. Hospitals work to reduce health care costs by offering preventive screening services, promote public health through wellness and nutrition initiatives, educate and train the next generation of medical professionals and conduct vital research aimed at preventing and treating disease. Even with national shortages, West Virginia hospitals have been able to expand the number of providers by nearly 20% between 2020 and 2023. These efforts reflect the hospitals’ enduring mission to strengthen the health and well-being of all West Virginians, regardless of ability to pay.
 While there are considerable challenges facing the state’s hospitals, there are encouraging signs for the future. State leaders, including the governor and Legislature, are actively working to attract new businesses and expand commercial employment opportunities across the state. These initiatives strengthen the state’s economic foundation and, more importantly, bring employer-sponsored insurance plans that offer more sustainable payments for hospital care.
While there are considerable challenges facing the state’s hospitals, there are encouraging signs for the future. State leaders, including the governor and Legislature, are actively working to attract new businesses and expand commercial employment opportunities across the state. These initiatives strengthen the state’s economic foundation and, more importantly, bring employer-sponsored insurance plans that offer more sustainable payments for hospital care.
The new federal Rural Health Transformation Program offers West Virginia a significant opportunity to address these challenges. The state’s application, submitted in November 2025, will provide West Virginia an opportunity to invest in additional economic development opportunities and wellness initiatives to reduce the cost of care, all while investing in the development of West Virginia providers and efforts to attract existing providers.